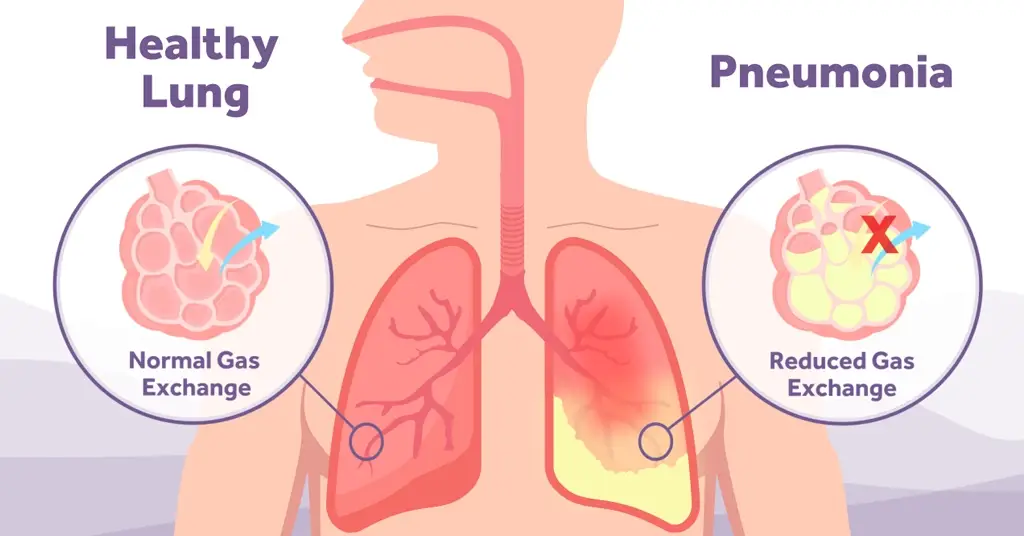
The importance of early mobilisation in ICU

With the rising cost of healthcare delivery and the increasing extended occupancy of hospital beds globally, many healthcare professionals, and indeed healthcare institutions, may look at ways to help shorten length of stay and improve patient outcomes.
The Society of Critical Care Medicine (SCCM) ICU Liberation Campaign (2018) aims to liberate patients from the harmful effects of pain, agitation, and delirium in the intensive care unit. Implementation of the ABCDEF Bundle showed significant and clinically meaningful outcomes, including improved survival, increased restraint-free care and reduced mechanical ventilation use, coma, delirium, ICU readmissions, with alterations in post-ICU discharge disposition.[1,2]
This quality initiative, also known as the ‘A2F Bundle’, aims to improve patient outcomes and reduce the risk of long-term consequences from an ICU stay which consists of the following individual elements:
A: Assess, Prevent, and Manage Pain
B: Both Spontaneous Awakening Trials (SATs) and Spontaneous Breathing Trials (SBTs)
C: Choice of Analgesia and Sedation
D: Delirium: Assess, Prevent, and Manage
E: Early Mobility and Exercise
F: Family Engagement and Empowerment
We will now focus on the element of early mobilisation – the practice of getting patients mobile as soon as possible post admission to critical care. This has been shown to be safe and feasible in both adult and paediatric populations. In adults, studies have shown that ICU-based early mobilisation decreases delirium, improves functional outcomes, and is cost effective.
Patients in the intensive care unit commonly develop muscle weakness. In part, this reflects loss of mechanical loading due to physical inactivity, bed rest, or immobilization.[3] Patients with critical illness can lose more than 15% of muscle mass in one week, and this can have long-term detrimental effects .[4]
Early mobilisation (EM) is the application of physical activity as early as the 2nd to 5th day after the onset of critical illness or injury [5] and is referred to as physical activity performed to the intensity that can bring about physiological changes. [6]
According to the World Health Organisation physical activity is defined as ‘any bodily movement produced by contraction of skeletal muscles that require energy expenditure’.[7] This can include exercise and other activities involving bodily movement.
Willigen, Z et al (2016) offered a Quality Improvement (QI) initiative in 2012 for mechanically ventilated medical patients in a general ICU. An integrated package of care involving two additional daily sessions of mobility therapy, in combination with minimal sedation, where possible, was offered. The aims of their project were to deliver early mobilisation and evaluate the impact on ICU length of stay, over a four-year period. Although explaining that EM is difficult to deliver, they made clear that there was a suggested reduction in length of stay in their patient cohort . [8]
EM can have significant benefits to patients and staff; these include reduced ICU-acquired weakness, decrease days of delirium, days on mechanical ventilation, improved functional recovery within hospital, improved walking distance at hospital discharge and reduced hospital length of stay. [9]
Although not exhaustive, recommended exercises include, passive and active range of motion, active side-to-side turning, exercising in the bed, transfers from the bed to the chair and vice versa, ambulation, and resistance exercises. [5]
It is acknowledged that not all patients in critical care can ambulate, this will vary based on the strength of activity, from passive stretching to active walking. It is important to set a daily activity goal for each patient based on the patient’s clinical status and resources available for support. Other methods of activity should be considered such as elevating the head of the bed, passive range of motion (ROM), manual turning, or dangling. It is worthy of note that non-ambulation for example may not be the only barrier to mobilisation.
The (SCCM) ICU Liberation Campaign (2018) has set out considerations of what to assess for when attempting to mobilise, these include neurological status such as level of alertness, cardiac stability and pulmonary assessment, for example ventilation and oxygenation needs. [1]
In their supplemental piece for My American Nurse, Amanda Veesart and Alyce S Ashcraft [10] list six potential barriers to early mobilisation namely; patient (or family) refusal due to patient pain and discomfort, large patient size, lack of personnel, lack of safe-patient handling and mobilisation equipment, lack of provider orders and failure to make mobilisation a priority.
At a time when hospitals are facing undue pressures perhaps the implementation of an Early Mobilisation Programme could help alleviate some pressures experienced in Intensive Care Units by way of improving patient mobility and mental wellbeing, freeing up beds more quickly through reducing length of stay, which in turn will allow for potential overall cost savings to the hospital.
Early mobility can be performed by any part of the interdisciplinary team including nurses, physio therapists, occupational therapists, or physicians and the full integration of quality initiatives such as the ABCDEF bundle can make ICU care more patient centred and holistic with the main goal being improving patient outcomes.
For patients that require respiratory therapies such as High Flow Oxygen Therapy and CPAP, the battery back up on the AquaVENT® FD140i device, of at least 60 minutes, enables healthcare professionals to safely mobilise around the bed space without an interruption in therapy.
[1] Devlin JW, Skrobik Y, Gélinas C, Needham DM, Slooter AJC, Pandharipande PP, Watson PL, Weinhouse GL, Nunnally ME, Rochwerg B, Balas MC, van den Boogaard M, Bosma KJ, Brummel NE, Chanques G, Denehy L, Drouot X, Fraser GL, Harris JE, Joffe AM, Kho ME, Kress JP, Lanphere JA, McKinley S, Neufeld KJ, Pisani MA, Payen JF, Pun BT, Puntillo KA, Riker RR, Robinson BRH, Shehabi Y, Szumita PM, Winkelman C, Centofanti JE, Price C, Nikayin S, Misak CJ, Flood PD, Kiedrowski K, Alhazzani W. Clinical Practice Guidelines for the Prevention and Management of Pain, Agitation/Sedation, Delirium, Immobility, and Sleep Disruption in Adult Patients in the ICU. Crit Care Med. 2018 Sep;46(9):e825-e873. doi: 10.1097/CCM.0000000000003299. PMID: 30113379. Clinical Practice Guidelines for the Prevention and Management of Pain, Agitation/Sedation, Delirium, Immobility, and Sleep Disruption in Adult Patients in the ICU – PubMed (nih.gov)
[2] Pun BT, Balas MC, Barnes-Daly MA, Thompson JL, Aldrich JM, Barr J, Byrum D, Carson SS, Devlin JW, Engel HJ, Esbrook CL, Hargett KD, Harmon L, Hielsberg C, Jackson JC, Kelly TL, Kumar V, Millner L, Morse A, Perme CS, Posa PJ, Puntillo KA, Schweickert WD, Stollings JL, Tan A, D’Agostino McGowan L, Ely EW. Caring for Critically Ill Patients with the ABCDEF Bundle: Results of the ICU Liberation Collaborative in Over 15,000 Adults. Crit Care Med. 2019 Jan;47(1):3-14. doi: 10.1097/CCM.0000000000003482. PMID: 30339549; PMCID: PMC6298815. Caring for Critically Ill Patients with the ABCDEF Bundle: Results of the ICU Liberation Collaborative in Over 15,000 Adults – PubMed (nih.gov)
[3] Chambers, Melissa A., Jennifer S. Moylan, and Michael B. Reid. “Physical inactivity and muscle weakness in the critically ill.“ Critical care medicine 37.10 (2009): S337-S346.
[4] Fazzini B, Märkl T, Costas C, Blobner M, Schaller SJ, Prowle J, Puthucheary Z, Wackerhage H. The rate and assessment of muscle wasting during critical illness: a systematic review and meta-analysis. Crit Care. 2023 Jan 3;27(1):2. doi: 10.1186/s13054-022-04253-0. PMID: 36597123; PMCID: PMC9808763. The rate and assessment of muscle wasting during critical illness: a systematic review and meta-analysis – PubMed (nih.gov)
[5] Castro-Avila, Ana Cristina, et al. “Effect of early rehabilitation during intensive care unit stay on functional status: systematic review and meta-analysis.“ PloS one 10.7 (2015): e0130722.
[6] Stiller, Kathy. “Physiotherapy in intensive care: an updated systematic review.“ Chest 144.3 (2013): 825-847.
[7] World Health Organisation. Physical Activity. http://www.who.int/topics/physical_activity/en/
[8] Van Willigen Z, Collings N, Richardson D, Cusack R. Quality improvement: The delivery of true early mobilisation in an intensive care unit. BMJ Qual Improv Rep. 2016 Dec 30;5(1):u211734.w4726. doi: 10.1136/bmjquality.u211734.w4726. PMID: 28090326; PMCID: PMC5223689. Quality improvement: The delivery of true early mobilisation in an intensive care unit – PubMed (nih.gov)
[9] Tipping, Claire J., et al. “The effects of active mobilisation and rehabilitation in ICU on mortality and function: a systematic review.“ Intensive care medicine 43.2 (2017): 171-183.
[10] Veesart, Amanda, and Alyce S. Ashcraft. “Get your patients moving—now!.“ The Essence of Nursing 10.5 (2015): 11-13.