Get in touch
We are committed to protecting and preserving the privacy of our visitors when visiting our site or communicating electronically with us.
Home > Perioperative Humidification
Perioperative humidification refers to the heating of gases that is delivered to the patient, around the time of surgery.
These gases are typically oxygen, air, or nitrous oxide, and once they are heated and humidified are delivered to the patient through a breathing circuit or mask. The practice of perioperative humidification is typically used to reduce the risk of complications and improve patient comfort before, during and after surgery.
The use of heated and humidified gases in the perioperative setting has become increasingly popular in recent years due the significant clinical benefits to the patient and to the surgical team.
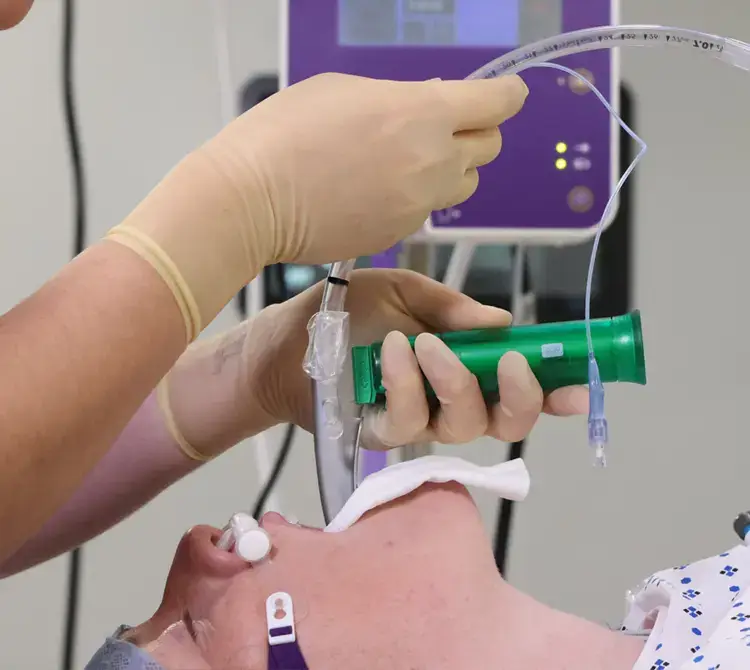
Extending the apnoeic window through hands-free pre-oxygenation.
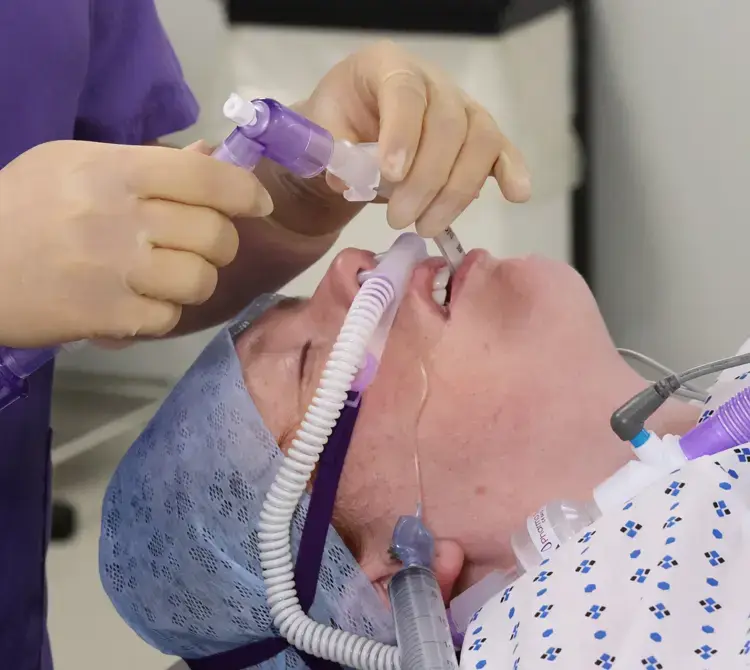
Improved visualisation during laryngeal surgery and improved biopsy samples.
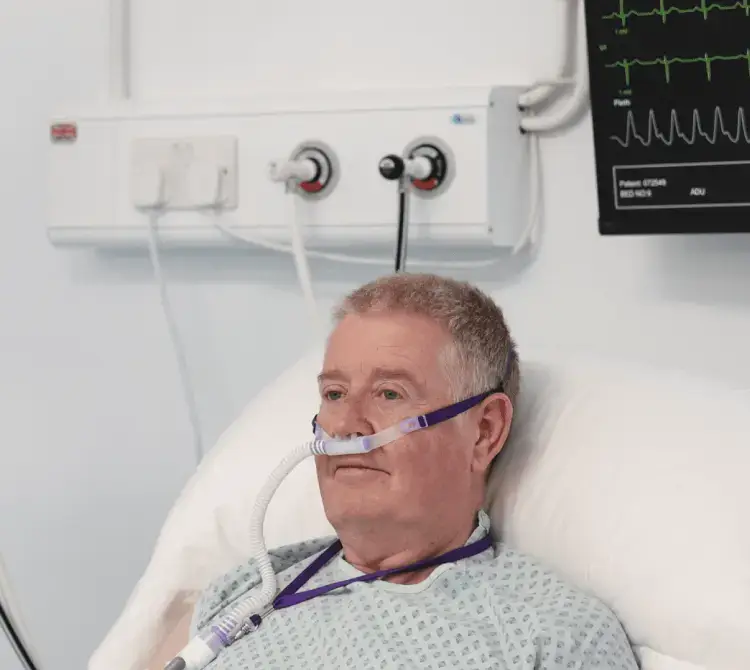
Reduced risk of complications and speedier return to normothermia.
Using pre-oxygenation to extend the apnoeic window (a finite time) to secure a definitive airway allows valuable extra time for intubation and an increased chance of a first-pass success (FPS) rate. This is particularly significant when dealing with a patient presenting with a difficult airway or at a higher risk of surgical complication.
During surgery, the airway can become dry due to a variety of factors, including the use of anaesthesia, the administration of dry oxygen through a breathing circuit, and the natural evaporation of moisture from the airway. When a patient’s trachea is intubated or a supraglottic airway device is placed in situ, the normal warming, humidifying, and filtering functions of the upper airways are bypassed. Artificially conditioning the gases by heating and humification replaces the lost functions of the body.
In theatre, general anaesthesia and inadvertent hypothermia is the most common perioperative thermal disturbance resulting from a combination of anaesthetic-impaired thermoregulation, the exposure of body cavities and blood loss, and exposure to a cold operating room environment.
Hypothermia, which is associated with increased morbidity and mortality in surgical patients, is the result of an internal core-to-peripheral redistribution of body heat that usually reduces core temperature by 0.5– 1.5°C in the first 30 min after induction.
The heated gases can help maintain normothermia by providing a warm and moist environment for the patient. The gases are heated to a temperature of 37-38°C, which is normal body temperature. The gases are humidified to a relative humidity of 100%, which helps prevent dehydration of the mucous membranes, therefore maintaining normothermia by reducing heat loss through the respiratory tract.
Medical equipment and circuitry to deliver heated and humidified HFOT for perioperative applications.
HFOT is delivered simply and efficiently using the AquaVENT® FD140i and an AquaVENT® HFOT circuit.
Delivering HFOT by this method creates the right combination for optimum results in your perioperative setting, supporting the patient at all points in their journey through theatre from preoxygenation to recovery.
We are committed to protecting and preserving the privacy of our visitors when visiting our site or communicating electronically with us.
THERAPIES
Armstrong Medical Ltd is a limited company registered in Northern Ireland
Wattstown Business Park, Newbridge Road, Coleraine, Co. Derry/Londonderry, BT52 1BS, United Kingdom
VAT Number: GB432578934
Company Number: NI025560