Postoperative Hypoxemia: Optimising Recovery with Oxygen Therapies

For this month’s blog, we will be taking a closer look at the challenges in postoperative care, specifically postoperative hypoxemia.
Postoperative hypoxemia: breathing easy after surgery
Hypoxemia is defined as inadequate tissue oxygenation due to either inadequate blood flow or arterial oxygen content 1. This can occur due to two main factors, firstly a disturbance in gas exchange caused by anaesthesia which can last for hours or days in the postoperative period. Secondly, an abnormality of control of breathing can manifest from episodes of obstructive apnoea rather than a decrease in respiration rate which can last for several days or nights postoperation2.
How common is postoperative hypoxemia?
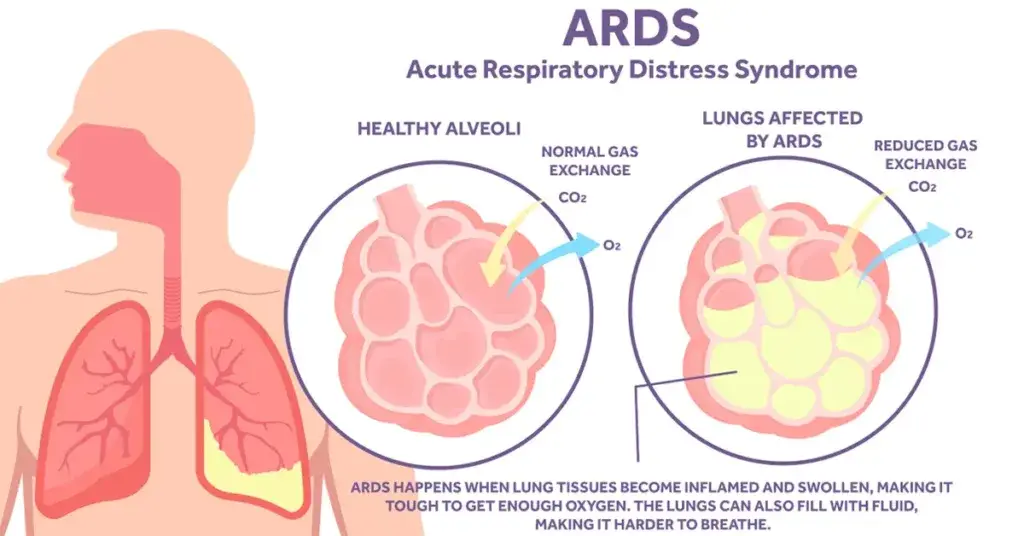
Postoperative hypoxemia is one of the most common complications after surgery, often due to atelectasis, ventilation/perfusion mismatch, or pulmonary oedema. Studies report an increase in mortality as high as 27% 3. Patients with postoperative hypoxemia can face longer hospital stays and extended rehabilitation. They can also experience compromised wound healing and other severe complications such as brain dysfunction, abnormal heart rhythms, and cardiac ischemia4.
Exploring the causes
Understanding the causes of postoperative hypoxemia is vital for its prevention and management. Several contributing factors can be categorised as follows:
Anaesthetic agents: Although imperative for surgery, anaesthetic agents can temporarily depress respiratory function. This may result in shallow breathing, hypoventilation, or even apnoea during the immediate postoperative period.
Pain medications: Opioid analgesics are frequently used for postoperative pain management. However, these medications can suppress respiratory drive and lead to hypoventilation, particularly when administered at high doses.
Surgical duration and positioning: The positioning of the patient during surgery is a pivotal factor of perioperative care. Specific positions can compress lung tissue, leading to reduced ventilation and impaired oxygen exchange. The duration of surgery can also increase the risk of hypoxemia.
Surgical site: Surgeries involving the chest or abdomen can significantly impact breathing mechanics due to their proximity to the diaphragm. Patients undergoing these procedures are more susceptible to postoperative hypoxemia5. In a study by Fernandez-Bustamante (2017)6 it was reported that of those undergoing abdominal, orthopaedic, and neurologic procedures, 19.6% required prolonged oxygen therapy and 17.1% developed atelectasis. These subjects also had significantly more ICU admissions, a longer ICU and/or hospital stay, and higher early mortality.
Comorbid conditions: Patients with pre-existing lung conditions, such as chronic obstructive pulmonary disease (COPD), and those with cardiovascular diseases are at a higher risk of postoperative hypoxemia. Similar risks apply to those who are morbidly obese, with a BMI>30kg/m.7
Age-related factors: The elderly often experience a decline in lung function, rendering them more susceptible to postoperative hypoxemia. Their reduced ability to compensate for oxygenation changes can exacerbate the condition.5
The role of oxygen therapy in the postoperative period
Various interfaces can be used to administer oxygen postoperatively including a simple face mask or low-flow nasal cannula. In recent years oxygen delivery via High Flow Nasal Cannula (HFNC) or Continuous Positive Airway Pressure (CPAP) has been increasingly used, as discussed in our June blog where we highlighted the work of Consultant Anaesthetist, Dr Jubil Thomas at Our Lady of Lourdes, Drogheda Hospital. We have also previously discussed in detail the benefits of heating and humidifying gases in the peri-operative setting in our Inspire Blog.
High Flow Oxygen Therapy (HFOT)
HFOT can deliver flows as high as 80L/min to achieve oxygen fractions as high as 100%, possible in single increments with the AquaVENT® FD140i. These high flows allow clinicians to meet or exceed the patient’s respiratory demand and provide a constant Fi02, therefore reducing the work of breathing8. There is also some evidence to show a varying degree of Positive End-Expiratory Pressure (PEEP)9. All of these can improve oxygenation for hypoxic patients, given the improvements in patient comfort, dyspnoea, respiratory rate, and gas exchange10. Oxygen therapy can also help with wound healing in the postoperative period, as recommended by the World Health Organization.11
In the context of high-risk patients undergoing cardiothoracic surgery, the use of High Flow Oxygen Therapy (HFOT) in the postoperative period has shown promise. It is associated with significant reductions in reintubation and the need for escalated respiratory support when compared to conventional oxygen therapy.4 Rochwerg et al. conducted a systematic review and meta-analysis, and their findings indicated a lower risk of intubation among subjects treated with HFOT compared to those receiving traditional oxygen therapy.
Continuous Positive Airway Pressure (CPAP)
In contrast, CPAP provides continuous delivery of pressure to the airways throughout inspiration and expiration. This can be delivered via a mask or helmet. CPAP is being increasingly used postoperatively to prevent respiratory complications such as atelectasis and increasing functional residual capacity, improving alveolar recruitment, and reducing work of breathing which in turn increases oxygenation.12 The application of CPAP following surgery increases oxygen levels and reduces the risk of postoperative reintubation and mechanical ventilation. Furthermore, CPAP lessens the frequency of apnoea and associated oxygen desaturation events post-surgery.12
Conclusion
Postoperative hypoxemia presents a challenge in postoperative patient care, necessitating a multifaceted approach. Hypoxemia, often a result of gas exchange disturbances and breathing control abnormalities, can lead to severe complications, including prolonged hospital stays and even mortality. Several factors contribute to its development and effective management and oxygen therapy options are crucial.
Oxygen therapies such as HFOT and CPAP, have gained prominence, showing improvement in oxygenation, and reducing the risk of reintubation. These therapies are also recognised for its potential to enhance patient comfort and facilitate wound healing.
Ultimately, the choice of oxygen therapy in the postoperative period should be tailored to the patient’s specific needs, considering risk factors and individual characteristics. These advancements in oxygen therapy techniques signify a positive shift towards better postoperative care, particularly for high-risk patients, enhancing patient outcomes and quality of care.
- Sarkar, M., Niranjan, N. and Banyal, P. (2017). Mechanisms of Hypoxemia. Lung India, [online] 34(1), p.47. doi:https://doi.org/10.4103/0970-2113.197116.
- JONES, J.G., (1990). Postoperative hypoxaemia: mechanisms and time course. Anaesthesia, 45(7), pp.566–573. doi:https://doi.org/10.1111/j.1365-2044.1990.tb14833.x.
- Arozullah, A.M., (2000). Multifactorial Risk Index for Predicting Postoperative Respiratory Failure in Men After Major Noncardiac Surgery. Annals of Surgery, [online] 232(2), pp.242–253. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1421137/.
- Chaudhuri, D.(2020). High-Flow Nasal Cannula in the Immediate Postoperative Period: A Systematic Review and Meta-analysis. Chest, [online] 158(5), pp.1934–1946. doi:https://doi.org/10.1016/j.chest.2020.06.038.
- Mazo, V., (2014). Prospective external validation of a predictive score for postoperative pulmonary complications. Anesthesiology, [online] 121(2), pp.219–231. doi:https://doi.org/10.1097/ALN.0000000000000334.
- Fernandez-Bustamante, A., Frendl, G. and Sprung, J. (2017). Postoperative Pulmonary Complications, Early Mortality, and Hospital Stay Following Noncardiothoracic Surgery. JAMA Surgery, [online] 152(2), p.157. doi:https://doi.org/10.1001/jamasurg.2016.4065.
- Gupta, H., Gupta, P.K. and Fang, X. (2011). Development and Validation of a Risk Calculator Predicting Postoperative Respiratory Failure. Chest, [online] 140(5), pp.1207–1215. doi:https://doi.org/10.1378/chest.11-0466.
- Rochwerg, B. (2019). High flow nasal cannula compared with conventional oxygen therapy for acute hypoxemic respiratory failure: a systematic review and meta-analysis. Intensive Care Medicine, 45(5). doi:https://doi.org/10.1007/s00134-019-05590-5.
- Luo, J. (2017). Positive End-Expiratory Pressure Effect of 3 High-Flow Nasal Cannula Devices. Respiratory Care, 62(7), pp.888–895. doi:https://doi.org/10.4187/respcare.05337.
- Oczkowski, S. (2021). ERS Clinical Practice Guidelines: high-flow nasal cannula in acute respiratory failure. European Respiratory Journal, [online] 59(4). doi:https://doi.org/10.1183/13993003.01574-2021.
- Allegranzi, B., Zayed, B. and Bischoff, P. (2016). New WHO recommendations on intraoperative and postoperative measures for surgical site infection prevention: an evidence-based global perspective. The Lancet Infectious Diseases, [online] 16(12), pp.e288–e303. doi:https://doi.org/10.1016/s1473-3099(16)30402-9.
- Pelosi, P. and Jaber, S. (2010). Noninvasive respiratory support in the perioperative period. Current Opinion in Anaesthesiology, 23(2), pp.233–238. doi:https://doi.org/10.1097/aco.0b013e328335daec.