Perinatal Excellence: Teamwork Matters

The term ‘team’ has been defined as “a group of people with complementary and overlapping skills, working together to achieve common goals” [1].
We know that good teamwork results in better outcomes and within the healthcare setting, good communication strategies and effective teamwork are essential for the delivery of safe, high quality patient care [2]. Increasingly, within the perinatal environment, it has been recognised that ‘non-technical’ factors, referring to the aspects of a situation that are outside of the equipment and environment, can have a significant impact on how certain procedures, such as neonatal resuscitation, are performed and therefore teamwork can have influence on infant outcomes [3].
The goal of a neonatal team
The environment of the neonatal care setting is one of the most complex, with perhaps the biggest range of specialties working within one ‘ward’ in the best interests of the baby. Neonatal Intensive Care Units (NICUs) are unique in their requirement to provide a broad range of care to a population of preterm babies with increasingly lower birth weights. A single ward, yet a medical ward, high dependency unit and intensive care space all in one. The patients under the care of the wider neonatal team are often very medically fragile, with complications associated with being born early. The goal is simple, from the moment a mum goes into preterm labour until the baby is safely discharged from the neonatal unit, a large multidisciplinary team must work together to ensure the best outcome possible.
Perinatal Optimisation
Day-to-day a multidisciplinary team (MDT) , working within their individual specialities to care for a preterm baby, are familiar with working in collaboration together. However, it is only in more recent years, when the benefits of and focus on perinatal optimisation have come to the fore, that the need for the neonatal team to collaborate and engage actively with the obstetric and maternity teams has been emphasised.
In the United Kingdom the British Association of Perinatal Medicine (BAPM) develop frameworks for practice and one of their more recent quality resources outlines their ‘Perinatal Optimisation Care Pathway’ (figure 1). BAPM has recognised that in order to successfully deliver this pathway there must be a “strong teamworking culture, high quality communication habits and pursuit of common goals within perinatal teams” [4] and that the interventions described in the perinatal optimisation pathway are “undertaken within a favourable quality context where the structure and processes support an optimal environment for delivering quality improvement” [4].
When perinatal teams work well together, they can provide a range of interventions throughout the antenatal, intrapartum and neonatal period to improve preterm outcomes. Key interventions such as antenatal steroids and magnesium sulphate, delayed cord clamping and making sure baby gets breast milk early are just some of the ways that a perinatal team can collaborate to give a preterm infant and their family the best chance of a good outcome. In situations such as neonatal resuscitation where the need to help baby breathe can often be unanticipated, effective teamwork is essential as many tasks need to be coordinated during this event [3]. Guidelines that govern newborn resuscitation globally, such as the Neonatal Resuscitation Program (NRP) regulated by the American Academy of Paediatrics [5] and the Neonatal Life Support (NLS) course regulated by the Resuscitation Council UK [6], have increasingly emphasised the importance of teamwork, recognising that teamwork has an impact on the effectiveness of neonatal resuscitation and that the outcomes of a baby after resuscitation have been shown to be more positive when the perinatal team demonstrate collaboration and good teamwork [7].
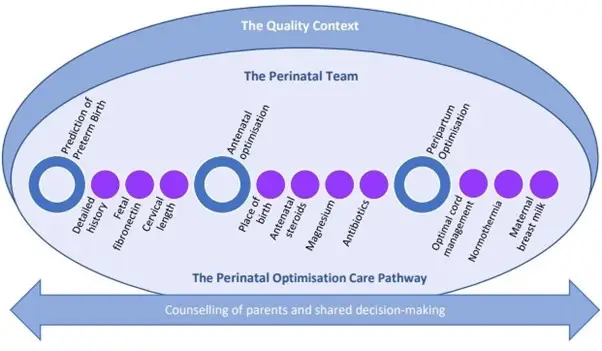
Figure 1: BAPM Perinatal optimisation (Perinatal Optimisation Pathway | British Association of Perinatal Medicine (bapm.org))
Conclusion
Events like neonatal resuscitation or stabilisation, following preterm birth, involve a team much bigger than the just midwifery or neonatology as standalone entities. The need for collaboration, good communication and effective teamwork will help ensure each baby has the best chance to experience optimal outcomes. Working effectively within a team may also benefit staff, by creating a shared purpose that promotes a feeling of social connection and a sense of belonging, which can lead to an increase in job satisfaction and reduced levels of burnout [8].
[1] Khawam, Ashley M., Toni DiDona, and Brenda S. Hernández. “Effectiveness of teamwork in the workplace.” International Journal of Sciences: Basic and Applied Research (IJSBAR) 32.3 (2017): 267-286.
[2] Leonard, Michael, Suzanne Graham, and Doug Bonacum. “The human factor: the critical importance of effective teamwork and communication in providing safe care.” BMJ Quality & Safety 13. suppl 1 (2004): i85-i90.
[3] Ediger, Krystyna, Marghalara Rashid, and Brenda Hiu Yan Law. “What Is Teamwork? A Mixed Methods Study on the Perception of Teamwork in a Specialized Neonatal Resuscitation Team.” Frontiers in Pediatrics 10 (2022).
[4] https://www.bapm.org/resources/building-successful-perinatal-teams-doc
[5] Weiner, G. M. M. D. “NRP Textbook of Neonatal Resuscitation.” (2021).
[6] Fawke, Joe, et al. “Newborn resuscitation and support of transition of infants at birth Guidelines.” UK Resuscitation Council, London (2021).
[7] Masten, Marjorie, et al. “Evaluating teamwork in the neonatal intensive care unit: a survey of providers and parents.” Advances in neonatal care 19.4 (2019): 285-293.
[8] Southwick, Steven Mark, and Frederick Seacrest Southwick. “The loss of social connectedness as a major contributor to physician burnout: applying organizational and teamwork principles for prevention and recovery.” JAMA psychiatry 77.5 (2020): 449-450.